Diabetes Week 2022
Diabetes - why does it affect Podiatry treatment?
Diabetes Week 2022 is coming up soon, so our latest blog will tell you a little about diabetes and your feet, and why it is such a big deal for Podiatrists.
Both Nikki and Anna specialised in the care of diabetic feet whilst working in the NHS and maintain a special interest in this area.
When someone has diabetes, then their body either doesn’t produce any insulin, doesn’t produce enough insulin, or they are unable to use the insulin that their body does produce, properly. Insulin helps the body to regulate blood sugar levels.
Prolonged periods of high blood sugars can contribute to damage to some parts of the body, mainly the kidneys, eyes, blood vessels and nerves.
So why is this so important to Podiatrists then?
The potential for nerve and blood vessel damage is the main cause of concern for Podiatry treatments.
A good circulation of blood to the feet is essential for keeping skin, nails, muscles, bones, and tendons etc healthy. There is a lot of artery between your heart and your feet that could be affected by damage due to diabetes (as well as some other things like smoking, cholesterol, and high blood pressure).
Nerve damage is also a potential risk factor in diabetics. You have several different types of nerves, but the ones which detect pain and pressure are of most concern. Your feet are very sensitive and for good reason, they take a lot of hammer over the years! If there is any nerve damage, then the body’s warning system isn’t working. For example, if your shoes rub and cause blistering, you need to be able to feel it to react. If you can’t feel pain or friction on your feet, especially if they are out of sight in socks and shoes, then you can end up with problems you aren’t aware of.
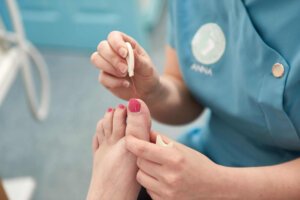
Poor circulation and loss of sensation from the nerves can lead to tissue damage on the feet. High pressure areas can be susceptible to breakdown, forming ulceration. There is also a higher risk of infection. Podiatrists carry out treatments taking all these factors into account.
The longer someone has diabetes and the less well controlled their blood sugars are, the more likely they are to develop complications.
Why your medical history is important to us.
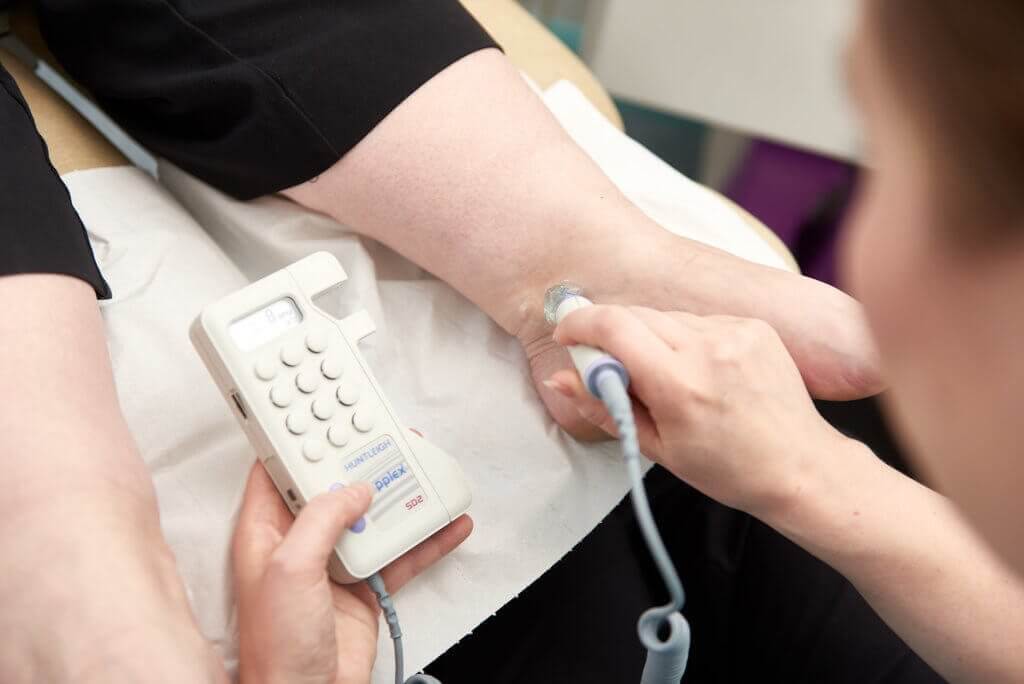
Lots of people ask us why we need to know someone’s medical history before we carry out any treatment. Podiatrists can screen patients for circulation and nerve damage with some very quick and painless tests. We use a doppler to listen to the quality of pulses in the feet to check for damage to blood vessels that may reduce circulation (see our blog on this here - https://roundhousepodiatry.com/circulation/circulation-problems-and-your-feet/ ) (it can also help us detect irregular heart rhythms which can be a risk for strokes). We use a small nylon filament to check for sensation too. The whole thing takes 5 minutes and helps us decide how our treatments may be affected and also if we need to refer to specialist interventions.
Good diabetic control and regular check-ups with your GP, nurse and Podiatrist will help to keep your feet in the best possible condition.
Remember – if you have concerns about your feet – find your local HCPC registered Podiatrist.
For more information on Diabetes - visit the Diabetes.co.uk website here
Anna Conway
BSc (Hons), MCPod, SRCh, PGcert Podiatry
Owner, Lead Podiatrist

